This paper is an easy read and really echoes what I and Dr. Harvey Risch, Peter McCullough, Robert Malone have been saying all along
Barouch does not try to impress with overly technical terms; bottom line is that routine boosting is dangerous, not viable (original antigenic sin); not risk-free, booster fatigue
Proposed Framework for Covid-19 Vaccine Boosters
‘The expectation that Covid-19 vaccines would prevent acquisition of infection and block onward transmission was based on initial data in 2020 (before the emergence of viral variants) that showed high neutralizing antibody titers and robust protective efficacy at peak immunity after mRNA vaccination. However, given the substantial waning of serum neutralizing antibody titers and the emergence of variants with increased transmissibility and antibody escape, it would be reasonable now to recalibrate goals for Covid-19 vaccines. Current vaccines may not provide high-level, sustained protection against infection or transmission with omicron, even after multiple boosts and also after the introduction of updated omicron-specific vaccines. Instead, the most important goal of Covid-19 vaccination should be to provide long-term protection against severe disease, hospitalization, and death from current and future variants.
Substack Alexander COVID News evidence-based medicine is a reader-supported publication. To receive new posts and support my work, consider becoming a free or paid subscriber.
Booster recommendations should therefore take into account not only peak neutralizing antibody titers but also durable prevention of severe Covid-19 disease. Such protection will probably require a combination of humoral and cellular immunity, with an emphasis on long-term rather than short-term immune responses. However, to date, the field has focused largely on short-term neutralizing antibody responses. The potential role of an omicron-containing booster is currently being explored, but a study in nonhuman primates showed that an omicron-specific mRNA vaccine was not better than the original mRNA-1273 vaccine for protection against omicron challenge.83 Early clinical studies have shown that boosting with bivalent mRNA vaccines containing both ancestral and omicron BA.1 spike immunogens induced peak omicron neutralizing antibody titers that were less than twice the peak titers induced by boosting with the original mRNA vaccines. Thus, clinical benefits of the updated boosters as compared with the current vaccines are not clear. Heterologous prime-boost (“mix-and-match”) regimens, which involve combinations of mRNA and Ad26 vaccines, are also being investigated as a strategy for improving the magnitude and durability of humoral and cellular immunity, as compared with either type of vaccine alone.52,84,85 In addition, early research on the development of pan-sarbecovirus and pan-betacoronavirus vaccines is under way.
Boosting every 4 to 6 months to maintain high serum neutralizing antibody titers may not be a practical or desirable long-term strategy. Boosting with mRNA vaccines is also not risk-free. Moreover, frequent boosting recommendations may worsen “booster fatigue” in the general population, given that to date only 47% of eligible persons in the United States have received any booster dose. Expert opinion on the benefits of frequent boosters remains divided, communications from public health authorities have been viewed as confusing and overpromising, and vaccine hesitancy remains a major challenge. Frequent booster recommendations may also distract from the critical goal of vaccinating the large number of unvaccinated persons in the United States and throughout the world and may further exacerbate global health inequities.
Plans for boosters should therefore be based on robust scientific data that show substantial and sustained increases in prevention of severe disease rather than on short-term increases in neutralizing antibody titers. Enhanced community engagement and implementation research may also reduce vaccine misinformation. Ideally, Covid-19 boosters should be recommended no more than annually and preferably less frequently, and a diversity of booster options should be available to the public. The use of vaccine platforms with improved durability would be highly desirable.
Conclusions
The Covid-19 pandemic appears to be transitioning from a hyperacute phase to an endemic phase. Current Covid-19 vaccines are less effective at blocking infection with the omicron variant than at blocking infection with prior variants, but protection against severe disease remains largely preserved. The primary goal of Covid-19 vaccines should be to provide long-term protection against severe disease, hospitalization, and death. It is therefore important for studies of Covid-19 vaccines and boosters to evaluate not only short-term neutralizing antibody titers but also durability of antibody responses, memory B-cell responses, and cross-reactive T-cell responses.’

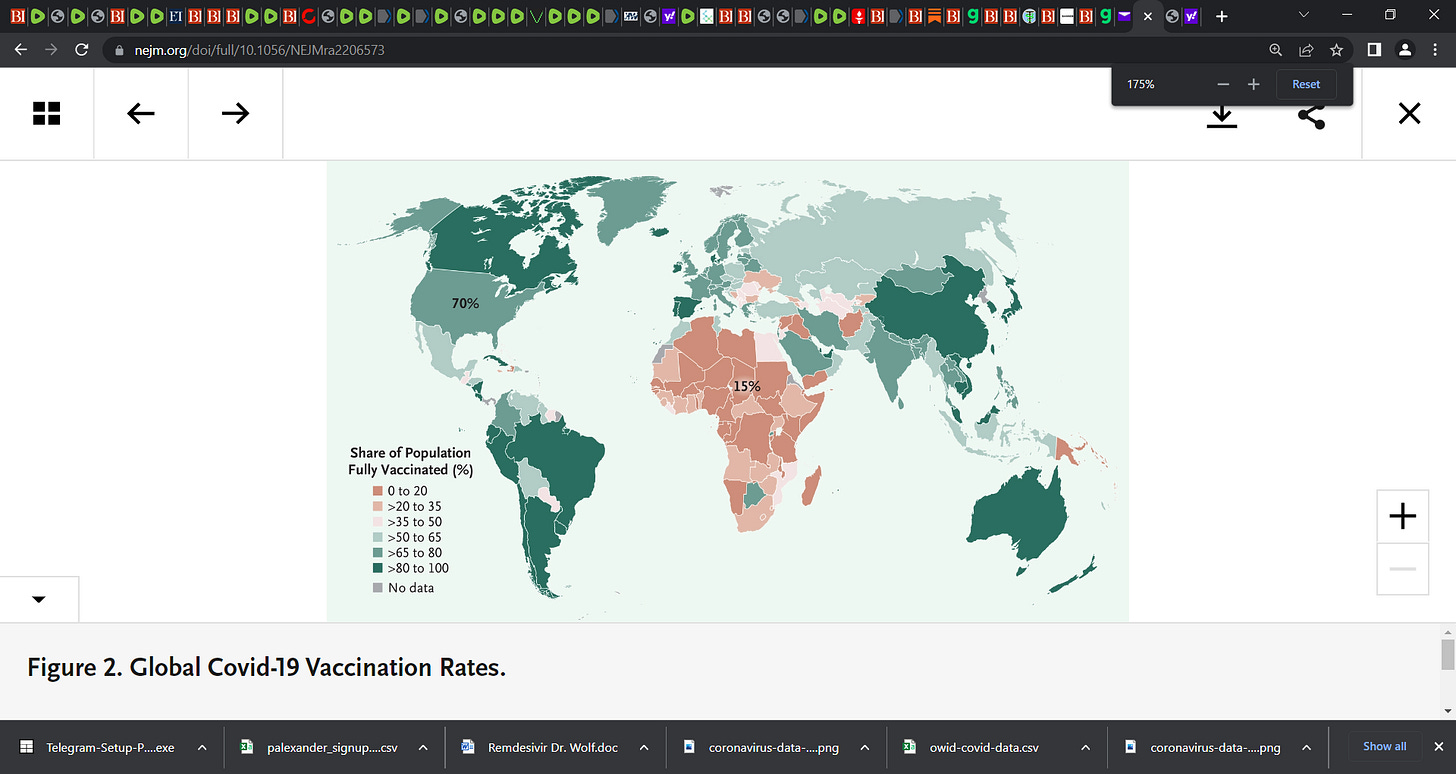
Source – https://palexander.substack.com/p/barouch-nejm-covid-19-vaccines-immunity
